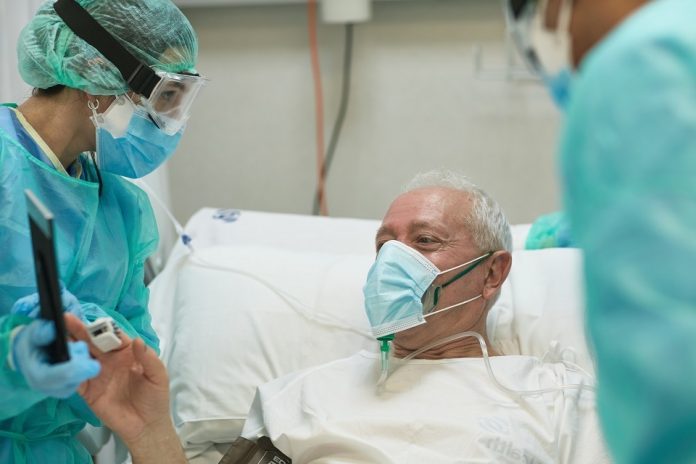
- COVID-19 patients are to receive second life-saving treatment for hospitalised patients outside of intensive care
- Thousands more lives could be saved as UK clinical trials show tocilizumab reduced the risk of death by 14% for patients on oxygen on top of benefits from dexamethasone
- Treatment will help reduce pressures on hospitals and improve outcomes for patients
Thousands more NHS patients who are hospitalised due to COVID-19 will be able to receive life-saving treatment tocilizumab, the government has announced.
The drug reduced the relative risk of death by 14% and reduced the time spent in hospital by 5 days when used for patients on oxygen and in addition to the corticosteroid dexamethasone.
The roll-out of this treatment could also contribute significantly towards reducing pressures on hospitals over the coming weeks and months.
Scientists discovered the drug was effective during the RECOVERY clinical trial, funded by the UK government through the National Institute for Health Research (NIHR) and UK Research and Innovation (UKRI).
Last month, the international clinical trial REMAP-CAP, also funded by the government, found that tocilizumab and sarilumab reduced the risk of death for patients when administered within 24 hours of entering intensive care.
The latest findings by RECOVERY, run by the University of Oxford, show a much larger group of hospitalised patients can also benefit from the drug if it is given to those outside of intensive care with oxygen deficiency and showing signs of worsening – meaning potentially thousands more lives could be saved.
Health and Social Care Secretary Matt Hancock said:
Today’s excellent news is further proof the UK is at the forefront of the global mission to find safe and effective treatments for this terrible virus.
I want to thank all those who have played a part in generating these tremendous results – from the British scientists and researchers behind the trial, to the thousands of patients who took part across the country.
We are working quickly and closely with colleagues across the health system and sector to ensure every NHS patient who needs this treatment should be able to access it – reducing further pressures on the NHS and potentially saving thousands of lives.
Deputy Chief Medical Officer Professor Jonathan Van-Tam said:
These results present another important advance in our fight against COVID-19 and are good news for patients and clinicians around the world – it’s a combination of both effective therapeutics and vaccines that will mean an end to this pandemic.
The data published today mean many more patients in hospital with COVID-19 will have access to a proven treatment, speeding up their recovery and reducing the risk of mortality significantly.
It’s because of the UK’s world-class clinical trials infrastructure, including NIHR infrastructure in NHS hospitals, and the generosity of UK patients to volunteer even though they are ill themselves, that trials like RECOVERY are able to deliver definitive evidence that will save lives, and I am hugely grateful to all those involved.
Professor Stephen Powis, NHS national medical director, said:
Throughout the pandemic where the NHS leads, the world has followed – from vaccinating the first patients outside of clinical trials to helping get dexamethasone into frontline care, and now to driving forward research on another breakthrough treatment.
I am immensely proud that the NHS is delivering another breakthrough treatment that will significantly increase the chances of survival for COVID patients being treated in England’s hospitals.
This is another positive development in our continued fight against the virus and alongside the roll-out of the biggest and fastest vaccination programme in our history, with over 10 million people receiving protection so far, we can start to look to the future with hope.
The government is working closely with the manufacturer Roche to ensure the drug is available across NHS healthcare settings.
This is the second treatment that RECOVERY, the world’s largest randomised controlled clinical trial, has found to be effective against COVID-19. It follows its discovery of the world-first treatment dexamethasone in June last year, which reduces the risk of death by 20% for patients on oxygen and 35% for ventilated patients.
RECOVERY has now found the benefits of using tocilizumab with dexamethasone are in addition to the benefits shown by dexamethasone alone.
Updated guidance will be sent to NHS trusts and clinicians on Monday, recommending they use this drug for hospitalised patients who may benefit from the treatment.
Throughout the pandemic, the government has supported British research with millions of pounds of funding for clinical trials into the most promising and innovative medicines in our fight against the virus, including for the RECOVERY trial.
The considerable success in large-scale clinical trials, like RECOVERY, is due to the UK’s world-class researchers, life sciences industry and research infrastructure, and the willingness of the public to volunteer, as well as existing NIHR infrastructure in NHS hospitals across the country.
With over 35,649 participants, RECOVERY is the largest randomised clinical trial anywhere in the world and will continue to trial other medicines, such as colchicine and baricitinib.
Marius Scholtz, Chief Medical Officer at Roche Products Ltd, said:
Today’s news is a positive step that increases our collective scientific understanding of COVID-19. It means that doctors across the NHS have access to a medicine that can help save the lives of hospitalised patients with severe COVID-19 and signs of inflammation. We are proud to have been part of a wide-ranging group, including academia, industry, the NHS, NIHR and government, that came together in an unprecedented way to fight this disease.
Background information
Tocilizumab (Roche), trade name RoActemra, is an anti-inflammatory monoclonal antibody, approved globally for the treatment of rheumatoid arthritis among other conditions.
Tocilizumab was added to the RECOVERY and REMAP-CAP trials in April.
The RECOVERY trial has demonstrated a 14% reduction in relative mortality and a 5-day reduction in hospital stays when tocilizumab is used in addition to standard of care. This is an absolute difference of 4%.
Previous results from the REMAP-CAP government-funded trial published on 7 January showed tocilizumab and sarilumab reduced the relative risk of death by 24%, when administered to patients within 24 hours of entering intensive care.
The RECOVERY trial investigates a different patient cohort to REMAP-CAP, meaning that its findings are relevant to patients in an earlier stage of the disease with oxygen deficiency, rather than those in ICU as for REMAP-CAP.
RECOVERY indicates efficacy for a patient cohort consisting of hospitalised patients who are receiving dexamethasone, are on oxygen, and have high levels of C-reactive protein (CRP) which is a marker of inflammation in the blood. Clinical guidance will be sent to trusts and clinicians shortly.
RAPID-C19 is the collaboration between the NHS, Medicines and Healthcare products Regulatory Agency (MHRA), NIHR and the National Institute for Health and Care Excellence (NICE), which will coordinate the advice to clinicians on appropriate use of tocilizumab.
A single UK-wide process to prioritise COVID-19 research as Urgent Public Health (UPH) research was established by NIHR early in the pandemic which prevented duplication of effort and ensured the UK ran large enough trials to get definitive answers to key questions. NIHR and the Medical Research Council (MRC) have worked together on this.
The NHS will ensure supply is maintained for current use for the drug’s current indications, such as rheumatoid arthritis.