Clap for NHS: Residents near St Thomas’ Hospital take part
Rupert Pearse, a consultant at a London hospital, said that while major incidents are usually over in a day, the relentless strain of the pandemic was “nothing like anything we’ve experienced before”. Pressure is likely to remain high until June and hospitals are already preparing for a third wave next winter, he said. The top medic also warned that the NHS must be ready for a surge in staff needing mental health support when they finally have time to reflect on what they have been through.
Speaking on behalf of the Intensive Care Society (ICS), Dr Pearse said “New admissions have slowed down and we are now discharging a similar number of patients as we are admitting. Things aren’t getting worse. They’re not quite getting better yet.
“Even if you just look at the patients we’ve got in hospitals at the moment, there are huge numbers, still more than 30,000 patients with Covid last time I looked.
“A lot of them will need months of care. We will certainly still have a lot of patients in hospital with Covid in June, even before you start to think about new patients coming in.”
There were 25,450 Covid-19 patients in English hospitals yesterday, including 3,275 in intensive care. And one in 10 major hospital trusts had no spare adult critical care beds last week.
A total of 15 out of 140 acute trusts reported 100 per cent occupancy of all “open” beds each day from January 25 to 31.
Following a steady fall in coronavirus cases, some ministers are said to be pushing for restrictions to be eased soon.Dr Pearse said NHS staff were “understandably anxious about how this is done – a big third wave would make things very hard”.
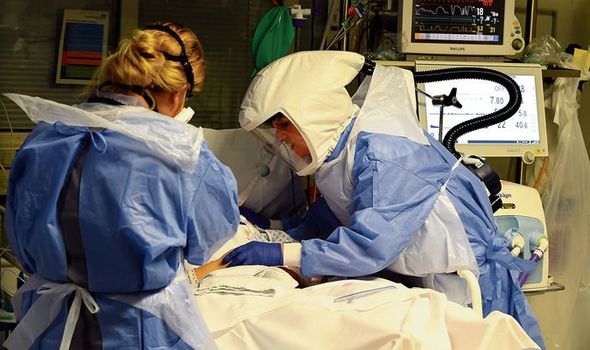
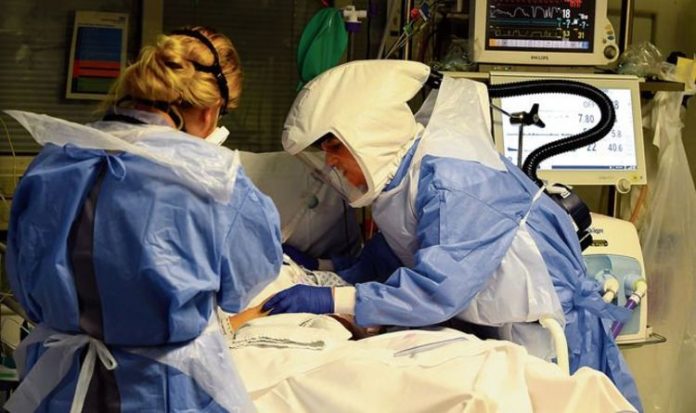
Intensive care staff working flat out in the second wave may be burying mental health problems (Image: Andrew Teebay/Liverpool Echo)
He added: “My eldest daughter missed her A-levels last year, my father-in-law is in his 80s and is awaiting urgent major cardiac surgery and that’s been delayed. All of those things, I want them to stop as much as everybody else does.
“But when we go to work and we see the continual extreme pressure… it creates a bit of a dissonance in our minds about what the best thing is.
“Ultimately I think most people in the NHS just want everybody to follow the guidance we’ve been given.” Asked how the pandemic compared to other high-pressure events, Dr Pearse said: “Major incidents are often almost back to normal within 12 hours and certainly by 24 hours.
“Even if you look at 7/7 or the London Bridge attacks, which my hospital was very badly affected by.
“The first wave of the pandemic lasted eight weeks before new hospital admissions calmed down.
“The second wave has been going on for more than three months and it’s only just peaked.

Hospitals are said to be already preparing for a third wave next winter (Image: Getty)
“To sustain that kind of emergency response for that long is not like anything we’ve experienced before, nothing like anything we’ve ever been trained to do.
“It’s just exhausting – that’s the only way to describe it.”
The ICS is concerned about the impact on staff mental health and says many are feeling anxious, having trouble sleeping and experiencing intrusive thoughts.
Dr Pearse fears many have not yet had time to process the last year.
He said: “I think you don’t really notice it in your day-to-day work until something happens that’s difficult – maybe things don’t work out well for a patient or there’s an argument – and we realise we’re much more vulnerable and fragile at those points than we normally would be. I suspect that a lot of this is kind of buried and people have hidden it in the back of their minds while they get on with this incredibly huge task.

Rupert Pearse says the strain of the pandemic is ‘nothing like anything we’ve experienced before’ (Image: NC)
“Only when that settles will we realise how many people have got mental health problems as a result.”
Post-traumatic stress disorder is a big worry, along with the risk of staff turning to unhealthy coping mechanisms such as problem drinking, Dr Pearse said.
He added: “As much as planning for how we catch up on cancer care and cardiac care for patients, how we look out for our NHS staff has to be part of that long-term planning. From what I’ve seen in my career, the NHS does take a lot of care of its employees but this is obviously a mammoth task for us.”
The ICS has launched an urgent appeal to support frontline staff. Its free well-being programme includes one-to-one psychological help, webinars and podcasts.
Dr Pearse said the prospect of a third wave was not helping, as hospital managers prepare for that eventuality. He said: “There’s always a third wave from these situations, it’s just a question of how big it is.
“If that third wave is very small we might be able to deal with it within our current establishment of NHS hospital and ICU beds but we need to have a plan in case it is very, very large. We can’t not plan.”
He added that with past outbreaks such as the 2009 swine flu pandemic, “it was a couple of years before the last patient left hospital”.
“Something on the scale of Covid we can expect, at the very least, to see a similar pattern,” he said.
NHS mental health director Claire Murdoch said: “Pressures on NHS staff have been intense and unrelenting, with 14,000 more Covid patients in hospital in the second wave compared to the first.
“It is crucial that hard-working staff are well supported and cared for, so we have invested £15million in support, including local mental health and well-being hubs, which are being set up across the country.”